Step 1 : Local Anesthesia
Level I Conscious Sedation Requirement
Patient safety is always our first priority. In Hong Kong there is no government regulation of Hair Transplant Center. We follow the American Standard of Office Procedure in administering local Anesthesia. We Adopt the MASSACHUSETTS MEDICAL SOCIETY OFFICE-BASED SURGERY GUIDELINES for your safety. According to these guideline there are 4 levels of office procedures - I, II, III, and IV. The safest office procedure amongst these 4 levels is Level I Conscious Sedation. This is exactly what we are using.
Level I office Procedure is also known as Conscious Sedation. Only local anesthesia is used without any intramuscualr or intravenous injection. This technique is catered for minor procedures including hair transplant. Amongst the 4 levels this is the safest level of sedation. Minimal oral relaxing medications are given before and during procedure. Chance of complications requiring hospitalization is uncommon. Without any drug induced alteration of consciousness, patients can response to verbal command. There is no interference with vital body functions
Pain Less Injection
The smallest 33G needle, together with various distraction techniques, are used to minimize any discomfort during the administration of local anesthesia.
Trained Staff
Our Staff has been trained to handle unexpected event and the use of resuscitation equipment. All assistant are required to complete a Certificate Course in Basic Life Support ( BCLS ). This Course is organized by Caritas Hospital Hong Kong
Resuscitation Equipment
In Level I Office Procedure there is no requirement for any Resuscitation Equipment. However to ensure your safety we have upgraded our equipment, which meets even the requirement of Level II and III:
• Oxygen source
• Airway equipment
• Positive pressure ventilation device
• AED (Automatic External Defibrillator
• Monitors for blood pressure, ECG, temperature
• Pulse oximeter
• Suction apparatus
• Emergency Drugs
Cases Not Suitable for Office Procedure
For safety reason we recommend patients with chronic diseases or immunosuppressed to have their procedure performed in hospital to avoid any unforeseen complicatons.
Step 2 : Donor Harvesting
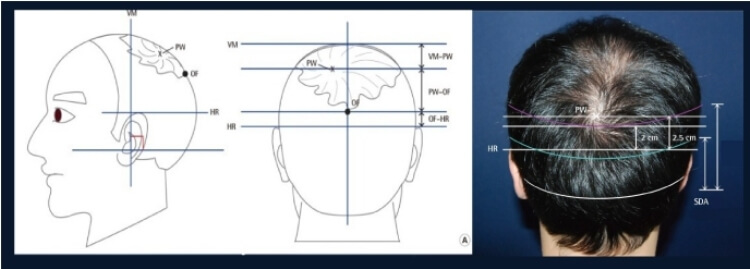
(Source of Picture) Donor supply is the ultimate limiting factor in hair transplantation for male pattern baldness (MPB) patients. According to Norwood's Classification, a man with advance Class VII balding would still have a rim of hairs at the sides and back of the head. This is labelled as the "Safe Donor Area" that is expected to be permanently covered with hair for a lifetime and therefore, provide permanent coverage when transplanted to the recipient area.
Defining the Safe Donor Zone
The boundaries generally extend from in front of the ears, around the temples, and to the back of the head. Exact mapping of this permanent donor area is still not possible. A rule of thumb is to forecast the maximum extent of alopecia progression). This may help to limit and confine the donor area. In young patients hair loss is progressive and unpredictable. Hair at the temples may recede back toward the ear, while balding area of the crown may dip quite low into the back of the head. A more conservative approach should therefore be adopted in defining the Safe Donor Zone. The most crucial of the safe donor area is the superior border. It was estimated to be about 5.5 to 6 cm from crown whorl (1). Hairs above this border are not recommended for transplant.
Donor Selection in FUE and ARTAS
Hair transplant surgeons have been trying to transplant the maximum-possible number of hair grafts in a single session to cover more of the recipient area. Many surgeons have frequently been in dispute about the appropriate standards for defining a safe donor area. FUE and ARTAS are known to require a much larger donor area when compared to Strip/FUT. It has been a great concern that some hair transplant surgeon chose to ignore this Safe Donor Zone when desperate for the number of grafts. This obviously viloates the true purpose of hair transplant.
Reference
1. J.H.Pak, et al. Predicting the Permanent Safe Donor Area for Hair Transplantation in Koreans with Male Pattern Baldness according to the Position of the Parietal Whorl. Arch Plast Surg. 2014 May; 41(3): 277–284.
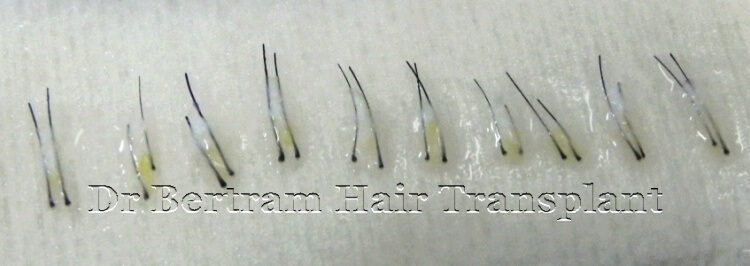
What is Follicular Unit
Scalp hair follicles were observed to bind together underneath the skin, emerging from the scalp in clusters or groups of 1-5 hairs in each pore. Each grouping of hair is called a "Follicular Unit" or "FU".
These naturally occurring follicular units of 1 to 4 hairs are properly transplanted to mimic the way hair grows in nature. Thousands of grafts can be transplanted in a single session to maximizes the cosmetic impact.
Normal Follicular Unit Density
The FU density varies amongst different ethnic groups, being highest in Caucasians and lowest in Africans
| Caucasian | Africans | Asians | |
|---|---|---|---|
| Hair Density | 200 / sq.cm | 160 / sq.cm | 170 ⁄ sq.cm |
| FU Density | 100 / sq.cm | 60 / sq.cm | 90 / sq.cm |
Ethnical Differences in Hair Characters
In order to provide hair transplant service to patients from different ethnic groups, we have studies in depth the differences in their hair density and characters
| Caucasian | Africans | Asians | |
|---|---|---|---|
| Hair Density | 200 / sq.cm | 160 / sq.cm | 170 ⁄ sq.cm |
| FU Density | 100 / sq.cm | 60 / sq.cm | 90 / sq.cm |
| Shaft Cross-Section | Oval | Elliptical | Round |
| Shaft Diameter | 0.07 mm | 0.06 mm | 0.08 mm |
| Hair Shape | Curly | Wavy | Straight |
| Length of Follicle | 4.5 mm | - | 5.5 mm |
Follicular Unit Density in Chinese Scalps
Usually the density is highest in the mid-occipit which is at the back of the head.
| Density (FU/sq.cm) | Front | Sides | Back | Average |
|---|---|---|---|---|
| Normal Men | 84 | 55 | 80 | 73 |
| Bald Men | 68 | |||
| Women | 87 | 54 | 72 | 72 |
| Bald Women | 69 | |||
Follicular Unit Ratio in Normal Chinese Scalps
The 2 Hair FU is the most common in Chinese, followed by the 1 Hair FU. 4- and 5- Hair FUs are very hard to find.
| Ratio (%) | 1 Hair FU | 2 Hair FU | 3 Hair FU | 4 Hair FU | Hair Graft Ratio |
|---|---|---|---|---|---|
| Men | 29 | 52 | 17 | 2 | 1.92 |
| Women | 33 | 49 | 16 | 2 | 1.87 |
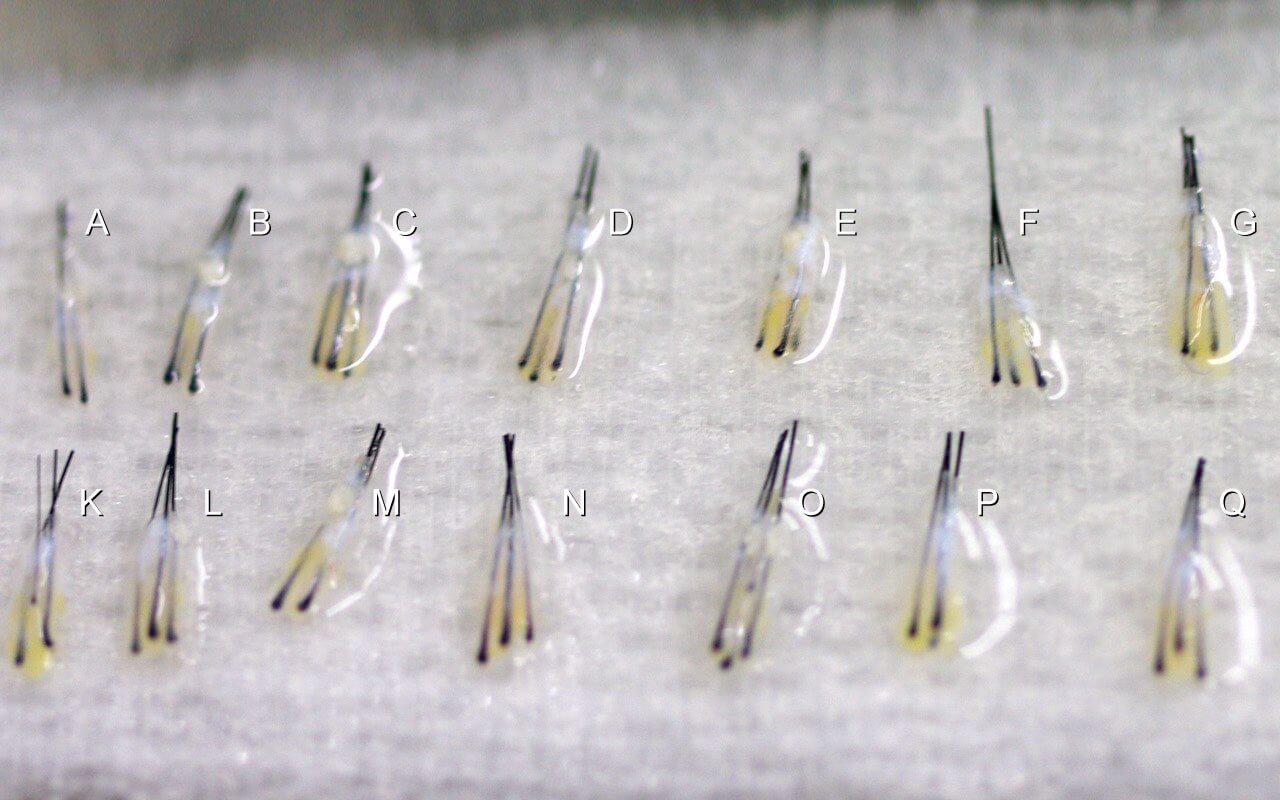
What is a Graft
Confusion arises when using different units to estimate the cost of a hair transplant procedure. Over 95% of hair transplant centers worldwide use "graft" as unit to estimate procedural cost. Advance in technology renders the smallest follicular unit to be used as graft. i.e. one graft = one FU. Nowadays 2,000 graft can easily be transplanted in one session.
Some centers however, limited by technique or manpower, may not be able to achieve such numbers. In order to sound good they instead use "hair" as unit. Telling a patient he had 2,000 hairs transplanted seems impressive but that's in fact just about 1,000 grafts. To avoid confusion ask clearly the unit for calculating cost.
Hair-Graft Ratio
Each individual will have a unique combination of 1-Hair FU, 2-Hair FU, 3-Hair FU. For a certain area the average number of hair per FU is known as Hair-Graft Ratio. The Hair-Graft Ratio is different amongst various Ethnic Groups. With a higher FU density and hair-graft ratio, Caucasians are more suitable for FUE.
Hair-Graft Ratio = Total Number of Hair ÷ Total Number of FU
| Caucasian | Africans | Asians | |
|---|---|---|---|
| Hair-Graft Ratio | 2.3 | 2.3 | 1.8 |
Objectives of Hair Transplant
1 : Hairline Restore
Restore the hairline and frame the face is the most important goal. In Asian males about 1,800 to 2,800 grafts can be harvested in first session. Asian males have about 5,000 to 7,000 usable donor grafts per life time. In Caucasian males 2,400 to 3,500 grafts are readily available due to their higher donor density. We do not recommend overharvesting as some donor hair should be reserved for the future.
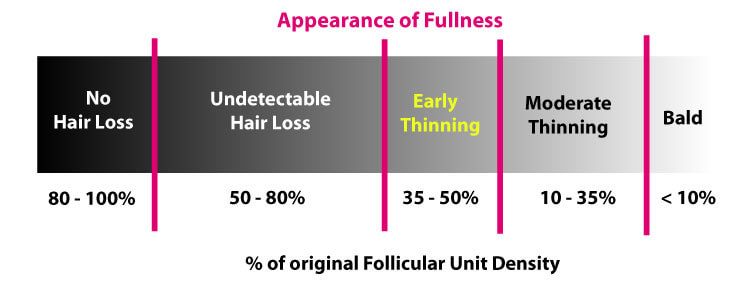
Objective 2 : Appearance of Fullness
A full head of hair appearance is Maintained until approximately 50% of the original hair volume is lost. Thinning is apparent when light is reflected from the scalp, creating a "see-through".
| Early Thinning | Moderate thinning | Bald |
|---|---|---|
| Losing 50% of hair | Losing 70% of hair | Losing 90% of hair |
| Scalp visible under bright lights or when wet | Scalp visible in almost all situations | No visible hair |
Illusion of Density - The 50 : 30 Rules
The human eyes are not very reliable sensors, especially in counting hair. The eyes cannot tell the differences when the density is above 50%. Consequently having 50% to 100% of the original density just look the same from a distance
The same principle can be applied when replacing hair. We only need to replace 50% of the original density to achieve an appearance of fullness. Spreading grafts over large area with density below 30% may look too thin for any satisfactory result
Factors to Consider
• Hair density
• Diameter of hair shaft
• Color contrast between hair and scalp
• Straight hair, wavy hair, or curly hair
• Amount of Existing hair
Normal Density ( Hair and Follicular Unit )
| Caucasian | Africans | Asians | |
|---|---|---|---|
| Hair Density | 200 / sq.cm | 160 / sq.cm | 170 / sq.cm |
| FU Density | 100 / sq.cm | 60 / sq.cm | 90 ⁄ sq.cm |
Recommended Follicular Unit Density in Hair Transplant
| Caucasian | Africans | Asians | |
|---|---|---|---|
| Minimal Density | 40 / sq.cm | 24 / sq.cm | 35 ⁄ sq.cm |
| Moderate Result | 45 /sq.cm | 30 /sq.cm | 40 /sq.cm |
| Dense Packing | 50 /sq.cm | 35 /sq.cm | 45 /sq.cm |
The grafts can be extracted either by removing a whole piece of scalp tissue (FUT); or extracted one by one (FUE). The choice of technique will depend on individual need. The doctor will discuss with you during the consultation.
FUE
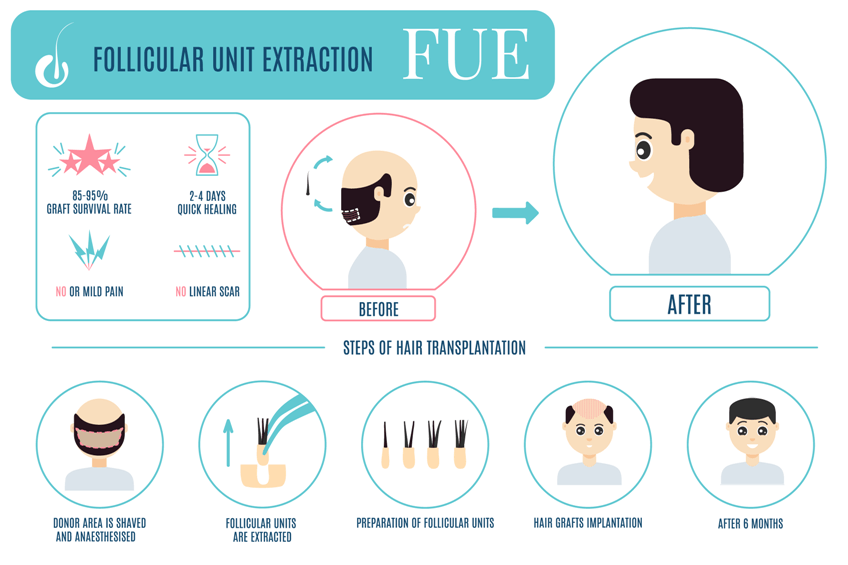
In FUE ( Follicular Unit Excision ) we use a size 1.0mm titanium round punch for Asian Hair and 0.8mm for Caucasian. This size keeps the grafts intact yet leaves minimal scar. Depth control is set to avoid graft transaction. We use bothe manual and automatic FUE, depending on your hair character. Every graft is extracted one-by-one carfefully not to damage any follicle ( READ MORE )...
FUT / Strip
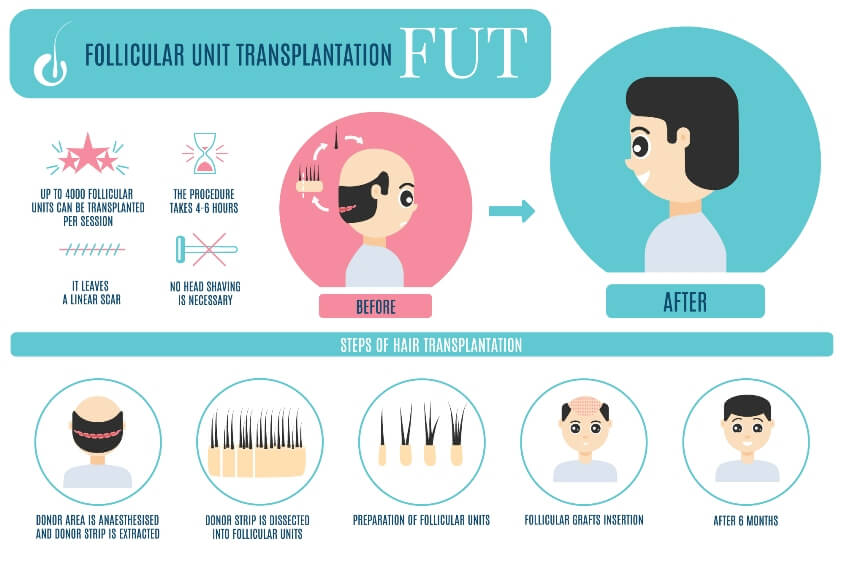
In FUT we dissect the strip with a single blade using magnified loupes. The blade is angled parallel to the hair follicles to minimize transection. Excision is made quite superficially with minimal bleeding. We routinely use the Trichophytic Technique as described by Dr Frechet. 2 layers suturing maximizes approximation and minimizes scar ( READ MORE )...
We select only good quality Grafts for transplant to ensure good result. Intact extracted grafts are sent to our assistants to trim all redundant tissues using 10X microscopic magnification. The follicular unit grafts are then sorted into 1-hair FU, 2-hair FU, 3-hair FUs. The intact follicles are stored in chilled saline enriched with ATP to ensure maximal graft survival.
Step 3 :Graft Insertion
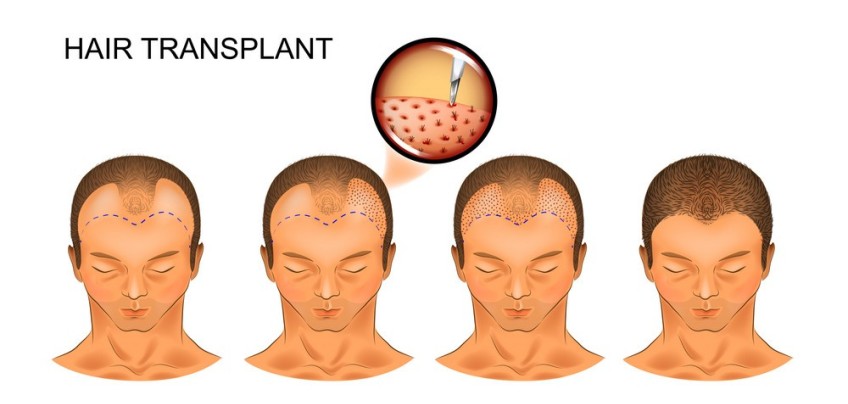
In the recipient site, small pockets in the skin must be created in order to accommodate the grafts. This step is called "Incision" or "Slitting". Slit sizes range from 0.7 to 1.2mm.
Incision is the most important step in the entire hair transplant procedures as the slits determined the final hair direction. Any mistake will render the result unnatural. The doctor has to study carefully the angle, direction, and orientation of your existing hair in the to be transplanted areas. Incision are then made to follow your natural hair flow. Loupes are worn to magnify the surgical field and to prevent damage to existing hair follicles.
Grafts outside the body has a limited survival time and must be implanted ASAP. Currently we are using 3 different Isertion Techniques depending on your hair characterd.
1. Forceps technique
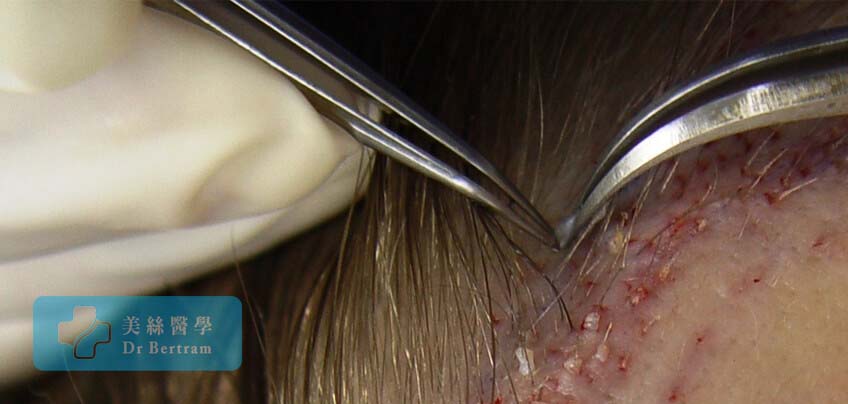
Fine tips jeweler's forceps are used to gently grasp the fat beneath the follicle to avoid trauma. It's our preferred method.
2. Implanter Technique
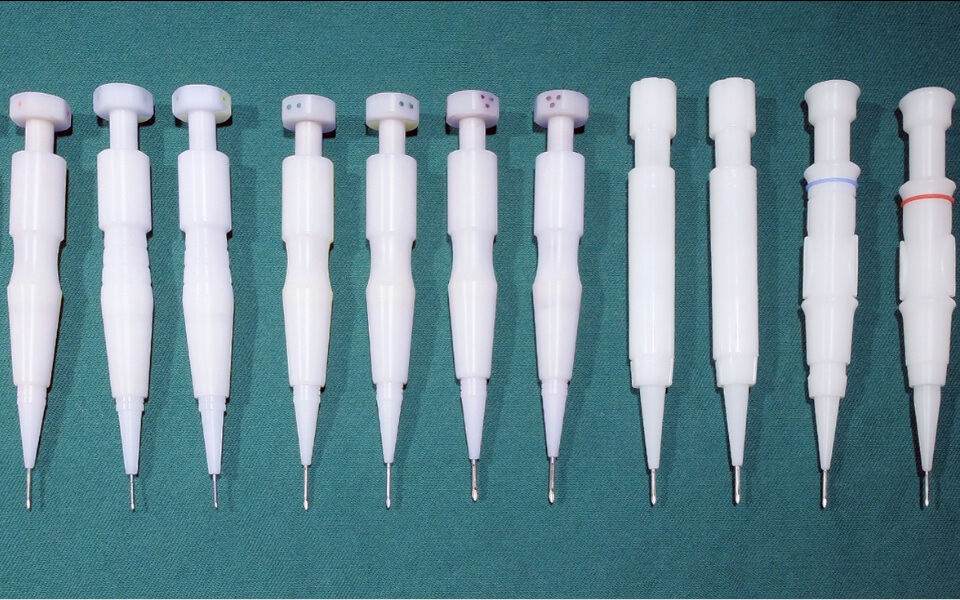
This is commonly used in Korea and Japan, especially for those using FUE. The follicle is first dragged into its metal tube before inserting the implanter into a slit. On withdrawal the graft is pushed out and left in the slit. We have abandoned implanter because of 2 reasons:
• More tissue trauma - the metal tube has thickness so holes larger than grafts have to be made
• Popping - insertion of an implanters will pop-up neighboring grafts, very difficult to dense pack.
3. Stick and Place
For dense packing we have to eliminate any empty spots between hairs. We keep about 10% of grafts at the end to fill in these spaces. After creating a slit a graft is inserted immediately. This technique of Stick and Place allows more grafts to be inserted per area.
Cautions
Hair transplant is a very safe procedure but not completely risk free. Here the possible Adverse Effects are listed together with our Protocols of Preventive Measure to minimize the risks.
Intraoperative Emergency
This is extremely rare in our level I office Procedure, when only local anesthesia and conscious sedation are used.
Our Protocol:
All patients are personally examine by our doctor
• General health, allergy, medication are all noted
• Careful selection of patients
• Close monitoring during procedure
• Standby equipment & well trained staff
• Doctor is in office at all time
Swelling Around the Eyes
During incision we inject tumescence to lift the scalp from the bone. After surgery when you resume the upright position this tumescence will drain down to your face and eyes, usually on the third day and lasts a week. This is harmless but unsightly and, once happens, nothing really helps.
Our Protocol:
Our tumescence is specially formulated to prevent swelling
• Use head band for 3 days except at sleep
• Avoid bending and eating salty food
• Massage any forehead swelling sideways
• Cool pack placed over the forehead for 15 minutes
Wound Infection
Our center infection rate is below 1%. We have stopped the routine use of antibiotic for over 1 year.
Our Protocol:
Selective use of prophylactic antibiotic in high risk patients (e.g. diabetes)
• Antiseptic hair wash before surgery
• Operate under an aseptic environment
• Follow-up on day 1 and 7 after surgery
• Meticulous wound care
• Avoid sweating from strenuous exercise the first week
• Frequent hair wash at home
• Prompt recognition and treatment
Numbness over the Transplanted Area
Making incisions temporarily traumatize the very superficial nerves. This may lead to numbness or pins-and-needles sensation. In a sense it is good as you won't feel any pain in the transplanted area. The course varies amongst patients, lasting from weeks to months. It does not affect your daily activities, felt only when touched. Full recovery is the rule.
Our Protocol:
The generous use of tumescence
• Set a depth guard to the blades to avoid too deep penetration
• Keep the entry angle of the blade rather flat to the skin
• Avoid overdose of local anesthesia
• Reassurance of full recovery
Pustules & Pimples
Small pimples or pustules are commonly found at 1 month and the 4 month after surgery. This is a benign condition and would not affect the final result. The old hair shaft detached from the graft would causes the following problems:
• Irritating the skin (foreign body reaction)
• Blocking the new hair from coming out
• Ingrown hair
Our Protocol:
Treatment is rather simple
• Squeeze out the pus and cleaned with alcohol or betadine
• Remove any hair spicule if loosen
• Maintain good hygiene with daily hair washing
• Avoid tight cap, hat, helmet, or hairpiece
• Apply antibiotic ointment as prescribed
• On rare occasion oral antibiotic may be needed.
Hair Loss around the Donor Wound
Shedding of hair below and above the sutured line, usually occurs 2-4 weeks after surgery. This is extremely unpredictable though the risk is higher if the wound is undermined and closed under tension. Full recovery is the rule but may take 4 months to re- grow.
Our Protocol:
Every patient is warned
• Keep at least 1 inch of hair at the donor area for cover-up
• Apply Minoxidil to the area before and after surgery may help
• Do not cut hair for a month after surgery.
• Reassurance of full recovery
Hair Loss around the Transplanted Area
This is the well known Shock Loss with shedding of existing hair within and around the transplanted area.Usually affects women with weak miniaturized hairs. Hair loss begins about 1 month and continue for 2-3 months. Re- growth may not be a 100%. Appearance improves when the transplanted hairs start to grow.
Our Protocol:
Warn every patient. Those unable to tolerate shock loss are refused surgery
• Select patients carefully, and exclude those with diffuse hair thinning
• Apply Minoxidil to the area before and after surgery
• In men shaving the transplanted area is the best prevention
• Avoid transecting pre-existing hair follicles during incision
• Avoid dense packing
• Women may wear a hair piece while waiting for hair re- growth.